The AGM100 is designed to identify hypoxemic patients like those with COPD or heart failure where the transfer of oxygen from the lungs to the blood is impaired. The Oxygen Deficit represents the degree of severity of gas exchange impairment and is more informative than PaO2 alone.
Assessments can be performed by anyone on the medical team with minimal product training. The procedure takes 2 minutes while the patient breathes at rest while wearing a pulse oximeter. The results include oxygenation, ventilation, and pulmonary gas exchange information that is useful throughout the continuum of care for cardiorespiratory patients.
Fast, non-invasive assessment of a patient's cardiorespiratory status.
Use with quick response team to help identify the chief problem
Monitor V/Q matching with Oxygen Deficit
Repeatable steady state analysis improves monitoring patients trending
Use Oxygen Deficit to help make home/observe/admission decisions
Use Oxygen Deficit to help predict the need for escalated care like supplemental oxygen
Identify hypoxic condition to improve treatment decisions
Use Oxygen Deficit for differential diagnosis e.g., NSTEMI vs PE
Determine the severity of cardiorespiratory patients using Oxygen Deficit
Identify or narrow the cause of diffuse chief complaints like shortness of breath or chest pain
Guide monitoring for residual shunt from the intra-operative period
Help early identification of atelectasis leading to hypoxemia
Support identification of post-anesthesia hypoventilation
Non-invasive confirmation of gas exchange efficiency before patient discharge
Help reduce avoidable postoperative pulmonary complications
Trend cardiorespiratory status in follow up visits




Assess patient arterial oxgygen, end tidal CO2 and end tidal O2 without leaving your office.
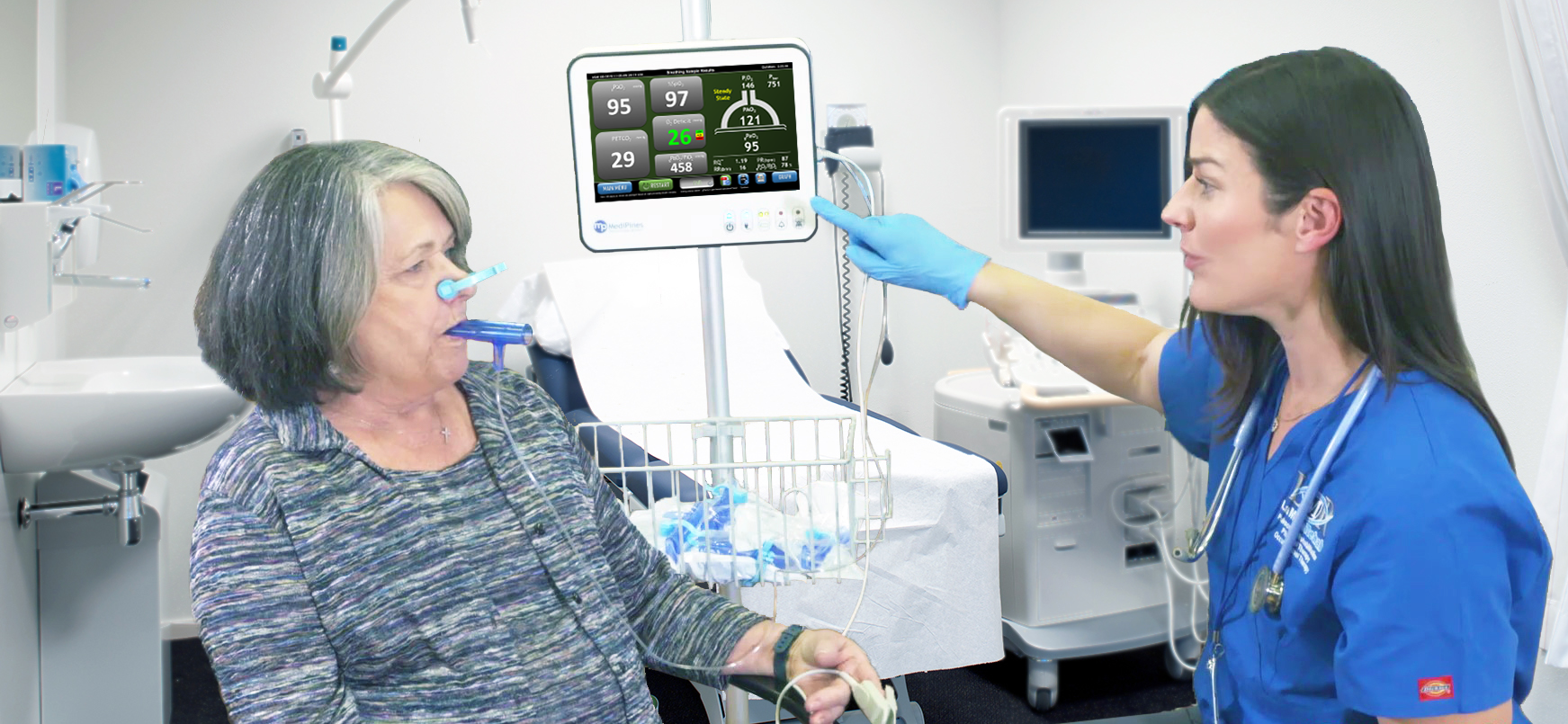
Reduce the number of patients sent to lab or ER for information like PaO2
Steady state analysis improves accuracy monitoring patients over time
Blood oxygenation, ventilation, and gas exchange simultaneously
Determine cardiorespiratory impairment severity using Oxygen Deficit
2-minute test allows assistant to make the measurement before being seen by the clinician
Automatic steady state recognition for repeatable result to test treatment effectiveness
Blood oxygenation, ventilation, and gas exchange simultaneously
Determine cardiorespiratory severity using O2 Deficit (non-invasive A-a gradient)
Establish clear baseline patient measurement prior to procedure
2-minute test allows MA to collect data and update chart before being seen by the MD
Automatic steady state recognition for repeatable result to test treatment effectiveness
Immediate results in office for faster clinical decisions
Fully reimbursable procedure
Reduce the number of patients sent to lab or ER for similar information
Objective, repeatable test improves monitoring patients over time
Use O2 Deficit to make home/observe/admission decisions
Use O2 Deficit to predict the need for escalated care like supplemental oxygen
Identify hypoxic condition and sources of hypoxemia to direct treatment
Use O2 Deficit for differential diagnosis e.g., NSTEMI vs PE
Determine cardiorespiratory severity using O2 Deficit (non-invasive A-a gradient)
Add clarity in diffuse chief complaints like shortness of breath or chest pain
Used with quick response team to help identify the chief problem
Use O2 Deficit as a surrogate for V/Q matching
Objective, repeatable test improves monitoring patients over time
Risk stratify surgical patients for postoperative pulmonary complications
Preoperative evaluation to determine oxygenation strategies
Establish baseline measurement prior to anesthesia
Monitor for residual shunt from the intra-operative period
Early identification of atelectasis leading to hypoxemia
Monitor for post-anesthesia hypoventilation
Confirm gas exchange efficiency before patient discharge
Reduce avoidable postoperative pulmonary complications
Confirm pharmacological effectiveness
Identify hypoxic condition and sources of hypoxemia to direct treatment
Complement ultrasound to determine severity using O2 Deficit (non-invasive A-a gradient)
Establish clear baseline patient measurement prior to procedure
Confirm degree of the blockage being treated
Identify secondary blockages with changes in gas exchange
Maintain stable V/Q matching before ending the procedure
Confirm pharmacological effectiveness before patient discharge
Use oxygen deficit to approximate pulmonary vascular pressures
Manage fluid buildup (edema) in heart failure to avoid readmission